PDF version [PDF:346KB]
Awareness of the Issue
The spread of Covid-19 is having a grave impact on our society. For example, in the Cabinet Office's "Quarterly Estimates of Jan.-March 2020 GDP (Second Preliminary)" the real GDP growth rate for the period was an annual negative 2.2% (year-on-year), but the average forecast of 12 private think-tanks puts the estimated growth rate for the April-June period at an annual negative 27% (year-on-year), and the Japanese economy looks set to sink to its worst level since the end of World War II.
On May 25, 2020, the Japanese government lifted the State of Emergency Declaration on the spread of Covid-19 across Japan, but with the reopening of social activities and economic activities, infections are once again spreading, especially around Tokyo.
Depending on the spread of infections, the government may once again issue restrictions on going out, or ask for voluntary restraint on business activities, but in this instance the economic loss will be immeasurable and the number of small and medium enterprises (SMEs) going bankrupt will likely rise sharply. In fact, the 2020 version of the White Paper on Small and Medium Enterprises (approved by the Cabinet on April 20, 2020) points to the "likelihood of concerns over financing difficulties in the accommodation and food service industry deepening for the next six months." According to the Financial Statements Statistics of Corporations by Industry (Ministry of Finance) for Fiscal 2018, cash deposits held by SMEs with capital of 10 million yen to 50 million yen only amount to around three months' worth of operating costs.
Is there a way to continue near-normal social and economic activities by utilizing the knowledge of economics? Addressing this issue requires collecting and putting together various kinds of expertise, but the most important requirement looks to be resolving "information asymmetry."
Currently, the number of confirmed cases in Japan is 42,098 people (as of Aug. 5, 2020), and this means that to begin with there are more people who are not infected. Yet why are the vast majority of people restricted from going out or asked to refrain from social and economic activities? This is because there is an "information asymmetry." For our part also, there are many cases where we ourselves cannot determine whether we have been infected or not. This is why we aim to lower the number of times we interact with other people by restricting ourselves or refraining from going out. Japan has thus far been successful in placing the so-called cluster control as its main strategy, but because the focus was on targeting the test subjects and tracing their contacts, the number of tests has been extremely low compared to other countries. But when normal economic activities re-open, if we are able to determine ourselves whether we have been infected or not by utilizing technology, the situation will change drastically.
This is why Professor Paul Romer of New York University, who is a Nobel Prize winner in Economics and a heavyweight of the American Economic Association, is recommending 20 million tests be conducted a day (https://roadmap.paulromer.net/). An infectious disease team in the United Kingdom is also recommending 10 million tests a day (https://ephg-covid-19.org/), while the Rockefeller Foundation proposes 30 million a day (https://bit.ly/2wWIxTC) and the Center for Ethics of Harvard University 50 million a day (https://ethics.harvard. edu/Covid-Roadmap). Quite coincidentally, from very early on (May 9, 2020), I and others constructed an online "Emergency Recommendation: Covid-19 V-shaped Recovery Project," and in the "Exit strategy" addressing expansion of Covid-19 we released an emergency recommendation to conduct 10 million tests a day.
The main message of the emergency recommendation is that "the most important aspect of balancing containment of the expansion of infections with social and economic activities is for all citizens to be able to regularly (around once every two weeks) find out, if so they desire, whether they have been infected with coronavirus, thereby creating a system, within six months at the latest, where people who continuously test negative feel safe to resume going out and work, and this is most crucial in going forward to the next step." Later, the Canon Institute for Global Studies and others released similar recommendations on expanding the testing system.
Is False Positive Really an Issue?
But expansion of the testing system in Japan is slow to move. One of the obstacles is the domestic debate on the "false positive issue." False positive refers to "testing positive when in fact the patient is not infected with novel coronavirus" and an index called "specificity" exists as a concept that demonstrates its accuracy (Table 1).
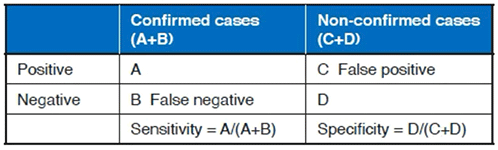
Specificity refers to "the percentage of accurately testing negative when not infected with the novel coronavirus," and the relationship "specificity = 1 – the percentage of false positive" generally holds. If specificity is close to 100%, false positive is generally zero. If specificity is 99.99%, false positive is a mere 0.01%. But when specificity is 99%, it causes major issues.
For example, when specificity of PCR tests is 99%, false positive exists by 1%, and if 14 million people (equivalent to the population size of Tokyo) are tested, even if the number of those infected is in fact zero, 140,000 people (= 1% of 14 million people) will test positive in the form of false positive cases. Even if they are false positive, if 140,000 cases are confirmed, it will exceed the medical capacities such as hospital beds and medical doctors who can treat the patients, and thereby will be highly likely to cause a collapse in the health system.
Therefore, in Japan, there are still voices that oppose the expansion of PCR tests citing the "false positive issue" as one of the reasons, but unless there are human errors such as sample contaminations, the specificity of PCR tests will never be 99% (false positive at 1%), and it is basically 100% (false positive at basically zero). PCR tests are outside the author's expertise, but this is a fact that came out of a series of study groups that were held with experts.
Several case studies that justify this will be introduced briefly. First is the case of Wuhan city in China. Infections in Wuhan had been contained for a while, but because newly infected patients were discovered between May 9 and May 10, 2020, after about five weeks of no new cases, all citizens in each of the districts of Wuhan were tested over the course of 10 days. Of roughly 9.9 million people, those infected with symptoms were zero, and 300 were asymptomatic. "Specificity = 1 – percentage of false positive," and it shows that even if all of the asymptomatic patients are false positive, the percentage of those that are false positive is less than 0.0031%, and therefore the specificity of PCR tests turned out to be more than 99.9969%.
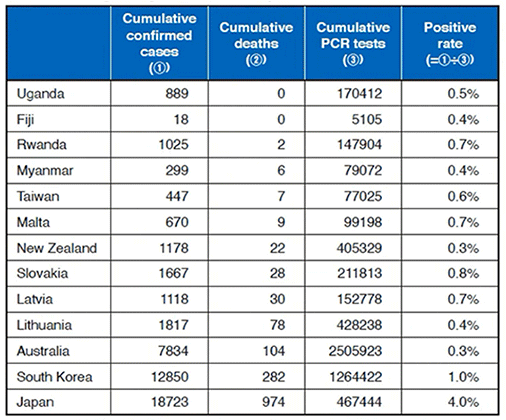
Chart 1 lists the rates of positivity in regions with low numbers of cumulative deaths (as of July 1, 2020), but false positives are part of the confirmed cases and therefore "percentage of false positive ≦ rate of positivity" holds (※1). As previously stated, "specificity = 1 – percentage of false positive" (※2), and for example, the rate of positivity in Australia is 0.3%, and therefore from ※1 and ※2 the specificity of PCR tests can be shown to be more than 99.7%. But included in the 0.3% rate of positivity must be those that are truly positive, and hence the specificity of PCR tests may be higher.
For example, let us look at a scenario where 20,000 tests are conducted twice a day, and suppose that there were 116 infected patients for the first test during a period when infections were spreading, and four infected patients for the second test when infections are being contained. The average rate of positivity is 0.3% (= 120 ÷ 40,000), but the rate of positivity for the first test is 0.58% (= 116 ÷ 20,000), and the rate of positivity for the second test is 0.02% (= 4 ÷ 20,000), and if specificity is to be estimated, including for those tests during periods when infections were spreading, true infected patients will also be counted and there is a possibility of mistaking specificity or judging false positive. In fact, it is desirable to estimate specificity from data when infections are being contained, and that can be read from data in Chart 2.
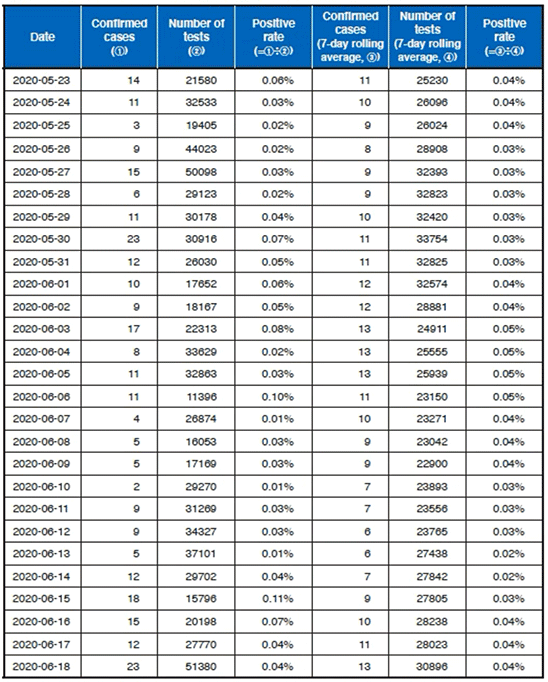
This chart shows the trends in the positivity rate of PCR testing in Australia for a given period (May 23 to June 18), and even when 20,000 tests, give or take, were conducted every day, there were many days when the number of confirmed cases was in single digits. If false positive exists around 1%, it means that it would not have been surprising to see around 200 false positive patients alone every day, but that was not the case. On the other hand, if the positivity rate was to be calculated using data in Chart 2, it is around 0.03%, and from ※ 1 and ※2 the specificity of PCR tests is generally around more than 99.97%.
Thus, "unless there are human errors such as sample contamination, the specificity of PCR tests is generally 100% (false positive is generally zero)" is the real truth, and politically opposing the expansion of the testing system based on the "false positive issue" basically does not hold.
Sensitivity or Frequency of Tests?
If false positive is not a major issue, the next issue that comes is "false negative." False negative refers to "testing negative when in fact the patient is infected with the novel coronavirus," and an index called "sensitivity" exists as a concept to demonstrate its accuracy.
Sensitivity refers to "the percentage of accurately testing positive when a patient is infected with the novel coronavirus," and generally "sensitivity = 1 – percentage of false negative" holds. If sensitivity is generally 70%, false negative is generally 30%, but if sensitivity is 40%, false negative becomes 60%.
Let us suppose there is a region with a population of 10 million and an initial infectious rate of 0.1%, how different will the trends be in the number of confirmed cases when tests are expanded for PCR tests with sensitivity of 70% and when tests are expanded for PCR tests with sensitivity of 40%? Chart 3 shows the results of a simplified simulation analysis using the SIR model, assuming a basic reproduction number R0 of 2.5, infectious period of 14 days, and specificity of 100%. The horizontal axis shows "the number of days since the initial condition" and the vertical axis shows "cumulative number of confirmed community transmissions."
The chart also compares four scenarios: "Basic scenario," "Test expansion 1," "Test expansion 2," and "Test expansion 3." "Basic scenario" sees infections expanding with no tests being conducted, while "Test expansion 1" shows a scenario where PCR tests with 70% sensitivity are conducted for a population of 10 million in 10-day intervals. Testing 10 million residents at 10-day intervals indicates building a testing system for 1 million tests per day.
"Test expansion 2" shows a scenario where PCR tests with 70% sensitivity are conducted for 10 million residents at five-day intervals, and "Test expansion 3" shows a scenario where PCR tests with 40% sensitivity are conducted at five-day intervals. Testing residents of 10 million at five-day intervals indicates building a testing system of 2 million tests per day.
Simulation analysis has been done based on these scenarios, and the overview is as follows. First, since the initial infectious rate is 0.1% and the population is 10 million, the number of confirmed cases in the initial stage is 10,000 people (= 10 million people × 0.1%), and the non-infected are 9.99 million people (= 10 million – 10,000 people). From the initial stage to day one, infected patients at the initial stage randomly transmit the virus at a basic reproduction number of R0=2.5 to non-infected people assuming a certain level of group immunity functionality. In this case, when infected patients are confirmed through regular PCR tests (sensitivity = 70% or 40%, specificity = 100%) conducted for the residents in the region via an expansion of testing, these confirmed patients are assumed to be quickly quarantined. Similarly, the number of confirmed cases on day two and forward is estimated based on data such as the number of confirmed cases on day one.
The results of this simulation analysis are shown in Chart 3. What we can learn from the results is that as trends in the number of confirmed cases show for "Test expansion 1," "Test expansion 2," and "Test expansion 3," the higher the "sensitivity" and "frequency" of testing, the lower the number of long-term cumulative confirmed cases. On the other hand, cumulative confirmed cases showed progressive increase for the "basic scenario" where no tests were conducted. This indicates the importance of the "sensitivity" and "frequency" of the tests.
(population of 10 million, initial infectious rate 0.1%)
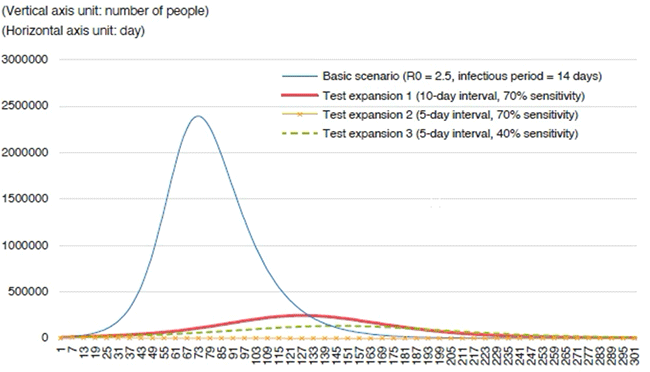
Which, then, is more important, the "sensitivity" (70% or 40%) or the "frequency" (10-day interval or five-day interval)? This can also be read from Chart 3. The chart shows that the number of confirmed cases during each peak at "Basic scenario" > "Test expansion 1" > "Test expansion 3" > "Test expansion 2," but the relationship "Test expansion 1" > "Test expansion 3" is particularly important. "Sensitivity" for "Test expansion 1" is 70% and "sensitivity" for "Test expansion 3" is 40%, and while the sensitivity of PCR tests for "Test expansion 3" is inferior to "Test expansion 1," by increasing the test "frequency" from the 10-day interval to five-day interval, the number of confirmed cases on the 50th day for "Test expansion 3" is at a lower level compared to "Test expansion 1." This indicates the possibility that "frequency" of PCR tests is more important than "sensitivity."
In preparing a mass PCR testing implementation system, the drive-through method of South Korea, the "regional PCR centers" of the Tokyo Medical Association, utilizing laboratories of dental doctors and medical doctors, and permission for pharmacies to do PCR testing as adopted in New York may all be utilized, but organizing PCR testing for voters at polling stations in the event of a House of Representative General Election may also be useful. In addition, in order to conduct mass testing, there is naturally a need to secure a great number of human resources and materials.
For human resources, medical experts such as doctors and nurses alone are insufficient in numbers to serve as testing personnel, and therefore there will be a need to allow testing to be conducted by non-medically licensed personnel also, who have gone through proper training, under the supervision of doctors or others. In this instance, the recommendation is to treat expansion of testing as part of public works, thereby prioritizing employing those who have lost jobs and development, perhaps more than it has up to now, and aim for urgent and speedy vaccine development, and such efforts should continue, but coming up with an "exit strategy" that relies solely on a successful outcome comes with huge risks. Thus, developing "treatment," not just new vaccines, is vital.
In other words, once infected with the novel coronavirus, if proper treatment can be developed at various stages of its symptoms through usage of effective existing medication or a combination of medications and prescribed quantities or frequency, and if the mortality rate can be brought down to a level equivalent or less than regular influenza, the issue of a trade-off between life and economy can be resolved and normal economic activities can be restored.
Regardless, what is important in addressing the expansion of Covid-19 is the final goal and a flexible strategy. To begin with, it is not appropriate to aim for 100% containment of the virus in a short period of time; rather, it is impossible. To uphold the mechanism of democracy and universal values such as freedom and basic human rights, and to gradually restore economic activities, it will be appropriate to aim for a 90% to 95% containment of Covid-19 by gathering public and private knowledge and expertise, and utilizing science and the latest technology led by the private sector.
As Chart 3 shows, the key to an exit strategy lies with "expansion of PCR tests." An incomplete strategy indeed is the worst, and it is important to be fully aware that aiming for a balance under such an incomplete strategy will, in the end, cause great harm to both.
This article first appeared on the November/December 2020 issue of Japan SPOTLIGHT published by Japan Economic Foundation. Reproduced with permission.
November/December, 2020 Japan SPOTLIGHT


