Nearly two years after the fight against COVID-19 began, I would like to discuss the balance between raising the vaccination rate, restricting economic activities, and expanding healthcare service capacity. We must be resolved to endure living with COVID-19 for several years even if vaccination becomes widespread. Therefore, we must consider different approaches to COVID-19 under two different timelines—COVID-19 containment measured in years, and intermittent outbursts of infection measured in shorter timescales.
One important fact concerning the long-term approach is that the vaccination rate is the predominant determining factor of the long-term, cumulative number of deaths from COVID-19 infection. According to a study conducted by University of Tokyo Project Assistant Professor Daisuke Fujii and University of Tokyo Associate Professor Taisuke Nakata (the results of their study were published in September 2021), and another study by Waseda University Associate Professor So Kubota (the results of his study were also published in September 2021), restricting economic activity in itself only has a minimal impact on the cumulative number of deaths. There is a simple reason for this fact, which is highlighted by Osaka University Specially Appointed Professor Fumio Ohtake in his essay (also published in September 2021), and outlined in the following paragraphs.
The mortality rate of COVID-19 is approximately 1% at present, but the rate could be reduced to a tenth of the present level (similar to the mortality rate of seasonal influenza, which is approximately 0.1%) if vaccination becomes widespread.. On the other hand, although restricting economic activities may slow the pace of infection, it is inevitable that nearly the whole population will be infected eventually.
That is because COVID-19 is so infectious that it is difficult to achieve herd immunity—the state in which the majority of vaccinated and recovered (immune) people act as a bulwark against the infection of the minority of unexposed and unvaccinated people. As a result, the mortality rate is the predominant determining factor of the long-term, cumulative death total from COVID-19 infection, while the status of society-wide vaccination is the predominant determinant of the mortality rate. In other words, to reduce the cumulative number of deaths, which is the most significant long-term cost of COVID-19, the most important goal for the moment is to maximize the vaccination rate.
On the other hand, restricting economic activities has the short-term positive effect of preventing the collapse of the healthcare system and avoiding the situation of being unable to save lives that could normally have been saved. Providing economic incentives (e.g., distributing product coupons and awarding gifts by lottery) will be an effective means of raising the vaccination rate. Announcing plans to relax the restrictions on activities by vaccinated people (e.g., easing of the restrictions on the holding of large-scale events and movement across prefectures) will also motivate more people to accept vaccination.
♦ ♦ ♦
In a phase of rapid infection expansion, we are confronted with the problem of the trade-offs between economic activities, general healthcare services, and providing care for COVID-19 patients. The fundamental causes of this trade-off are a shortage of healthcare resources (e.g., personnel and hospital beds) and a supply-demand imbalance regarding those resources.
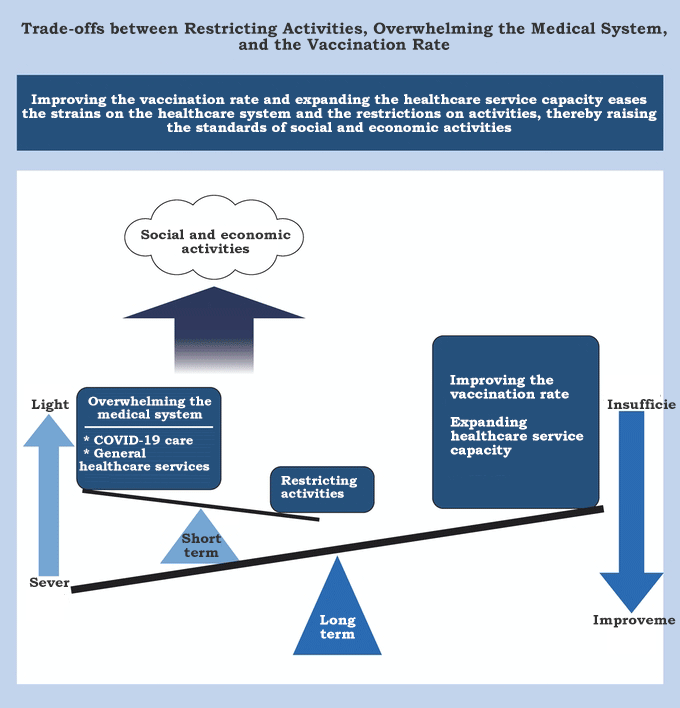
According to the abovementioned analysis by the Fujii-Nakata group and an essay by Asako Chiba (published in August), a postdoctoral fellow at the Tokyo Foundation for Policy Research, it is estimated that if the capacity of COVID-19 care (in terms of the number of hospital beds) is tripled from the present level, it is possible to return economic activities to the pre-pandemic state without allowing the healthcare system to collapse.
As for the shortage of healthcare resources, it is essential to prepare for the onset of a sixth wave of the pandemic and a subsequent explosion of infection by systematically opening oxygen stations and stations for patients waiting for hospitalization and by converting gymnasiums and other facilities into emergency healthcare facilities by equipping them with beds and oxygen supply devices.
With respect to the supply-demand imbalance regarding healthcare resources, it is necessary to develop a system for efficiently reassigning doctors and nurses between general healthcare and COVID-19 care. As a result of the revision of the Act on the Prevention of Infectious Diseases and Medical Care for Patients with Infectious Diseases in February 2021, governors have been empowered to require healthcare institutions to provide personnel and beds and to disclose the names of institutions that have refused to comply. It is important to strictly enforce the law and to consider revising it once again, if necessary.
During the explosion of infection in the fifth wave of the pandemic, some emergency healthcare facilities, such as oxygen stations, refused to accept patients even though there were vacant beds, citing shortages of nurses and other staff. Unadmitted patients were forced to depend on self-care at home and were thus exposed to the risk of a sudden change in their health conditions. Despite the staff shortages, emergency healthcare facilities should have continued to accept patients up to full capacity because staying at such facilities would have enabled more efficient response to a sudden change in conditions than depending on self-care at home.
Presumably, one factor behind that situation was unwillingness on the part of frontline workers to be held liable in the case of a sudden change in conditions at an undermanned facility. It is necessary to develop rules that exempt frontline workers from such liability in the case of a sudden change in conditions at an emergency facility and to have the government bear full responsibility in such cases , for example.
♦ ♦ ♦
It is essential to make constant efforts to resolve such shortages and imbalances of healthcare resources, but during an explosion of infections, it is also necessary to appropriately evaluate the trade-off between economic activities, COVID-19 care and general healthcare services and to restrict activities in these three fields in a "fair" manner.
When considering the trade-offs, it is not appropriate to compare the monetary losses related to economic activities against the value of human lives lost in the pandemic, but there is no difference in value between deaths in the form of suicides that were attributable to economic difficulties or mental problems associated with COVID-19, and deaths from COVID-19 infection.
The Fujii-Nakata group compared the numbers of additional suicide deaths associated with the COVID-19 crisis and deaths from COVID-19 infection in terms of the number of years of life expectancy lost. On a cumulative basis, for the period until the end of August, there was not a significant difference between the two categories of deaths, with the total number of years of life expectancy lost at 190,000 years in the case of suicide deaths, which included the deaths of many young people, and around 170,000 years in the case of the deaths from COVID-19 infection, which included the deaths of many elderly people) (the analysis results were published in October).
If we consider the degree of restriction that occurs with respect to each economic activity, COVID-19 care, and general healthcare services, it is theoretically possible to apply the "marginal principle," which represents the relationship between trade-off factors in economics.
From the comparison between general healthcare services and COVID-19 care based on the marginal principle, we may argue as follows. In the trade-off between those two factors, "the number of additional lives that may be saved through additional expansion of the capacity of COVID-19 care" should be equal to "the number of additional lives that may be lost due to the imposition of additional restrictions on general healthcare services." As all lives are equal in value, it should be desirable to adjust the degree of restriction on general healthcare services to ensure that the numbers of additional lives saved among COVID-19 patients and among patients receiving general healthcare services are balanced.
Sometimes, the idea of "expanding the capacity of COVID-19 care to an extent that does not affect general healthcare services" is advocated by people involved in healthcare policy planning. However, that idea means making distinctions between lives (giving precedence to the lives of patients receiving general healthcare services over those of COVID-19 patients), so I do not believe that making policy decisions based on the idea is appropriate.
The marginal principle regarding human lives can also be applied when policymakers determine the degree of restriction on economic activities. According to the marginal principle, the degree of restriction on economic activities should be determined in such a way that the number of additional suicide deaths associated with the COVID-19 crisis that may result from the adjustment of restrictions is balanced with the number of additional lives saved among COVID-19 patients.
To ensure fairness while restricting everyday lives and economic activities through policy measures, it is necessary to make policy decisions in such a way as to ensure that each life lost to COVID-19 infection and each life lost to COVID-19-related suicide are treated equally in terms of their value.
* Translated by RIETI.
October 19, 2021 Nihon Keizai Shimbun


