The caregiving workforce in the US will have to dramatically expand to meet the needs of the ageing population. This column argues that less-educated immigration could partially solve the problem. Using data from 1980 to 2017, the authors show that immigration increases the supply of home care for the elderly in the US and reduces its cost, while at the same time improving the quality of care for those who live in institutions.
The populations of advanced economies are ageing. In the US, the number of people age 85 and up will be more than double to 14.4 million by the year 2040 (Note 1). A substantial fraction of those will have some type of disability (see Figure 1) and will likely need some form of care or assistance with daily tasks. A majority of older Americans would prefer to ‘age in place,’ in other words, to live in the community rather than in an institutional setting (Binette and Vasold 2018). Families may be especially hesitant to use institutions now, given that nursing home residents account for one in six (over 145,000) deaths from the Covid-19 pandemic in the US (Note 2). Barczyk and Kredler (2018) find that the US relies on informal care more than most advanced economies. However, changing demographics and the burden on family caregivers make reliance on informal family-based care unsustainable. Over 800,000 Americans are already on waiting lists for formal home-based care and other supports for ageing in place (Note 3).
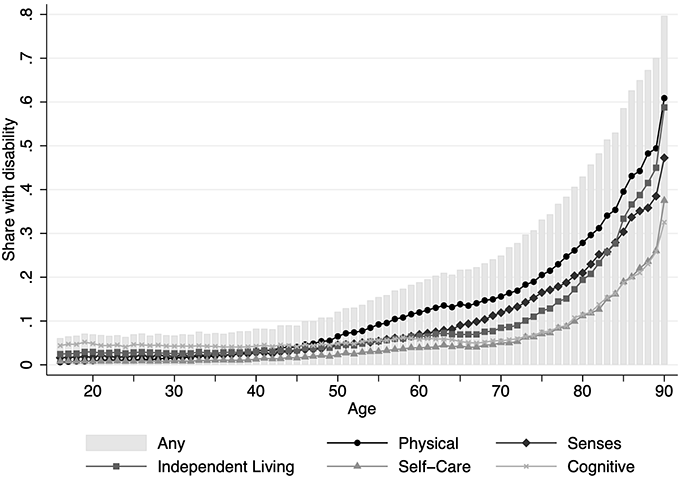
Note: Figure 1 depicts the share of all individuals in the U.S. (native and foreign-born) at each age who reported any or a particular disability. The right-most data point in each series combines those ages 90 and older due to top-coding in the data.
Expanded immigration could be part of the solution. Immigrants disproportionately work in occupations that facilitate ageing in place. More than a quarter of home health aides and nearly half of housekeepers and gardeners were born outside the US (see Figure 2). And prior research shows that immigration can facilitate household production. For example, Cortes and Tessada (2011) show that high-income women work more outside the home when there are more immigrants in the area, presumably because they provide childcare and household services.
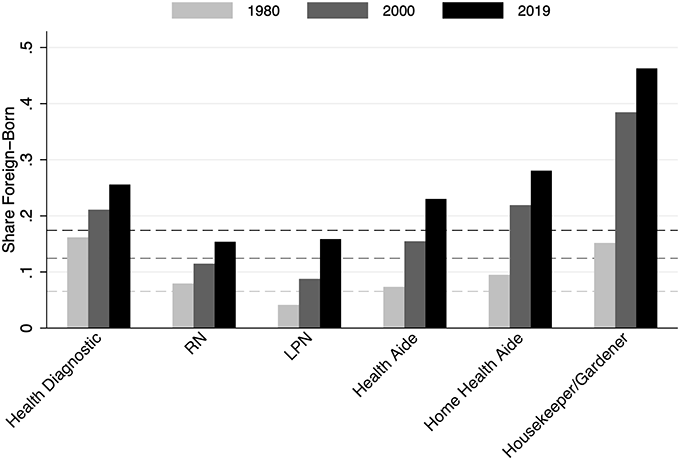
Note: The population represented consists of employed workers aged 16-64. Dashed lines indicate the share of this population (regardless of occupation) who are foreign-born. Bars indicate the share of employed workers aged 16-64 in certain occupations who are foreign-born. Colors of the dashed lines and bars designate years. Home health aides is a subset of health aides and are defined using a combination of the Census and ACS occupation and industry codes.
Does immigration similarly facilitate elderly caregiving in the home? It appears so. In a new paper focusing on the US between 1980 and 2017, we see the propensity for older Americans to live in an institution at any given age is on the decline (Butcher et al. forthcoming). Nursing home use fell even more quickly when there were increasing numbers of immigrants living in the local area. Other recent research also corroborates this finding (Mockus 2021).
There is a chicken-and-egg problem that needs to be addressed before we can claim a causal link between immigration and a decline in institutionalisation. For example, perhaps immigrants chose destinations where there were many older people choosing to age in the community and therefore many home health aide jobs were available. We use a method previously developed by Bartel (1989), Altonji and Card (1991), and others, which takes advantage of the fact that, especially between 1980 and 2000, immigrant country-of-origin networks are important predictors of where within the US immigrants choose to reside.
We use 1970 historical settlement patterns, coupled with more recent US immigration trends, to predict where immigration would grow the most between 1980 and 2000. For example, because Los Angeles had more Mexican immigrants in 1970 and Boston had more Italian immigrants, Los Angeles would be predicted to have higher immigration growth in subsequent decades because of the relative increase in inflows from Mexico. Using this ‘shift-share’ method, we see that areas with more predicted immigration growth have lower institutionalisation rates among the US-born. This approach accounts for local labour market conditions and therefore increases the likelihood that immigration causes lower institutionalisation, rather than the other way around.
How does immigration enable older Americans to stay out of institutions? The short answer is that there are more workers to provide support. The supply of caregiving and related services expands, and the cost goes down when the number of less-educated immigrants goes up. We see this in wages and shares of the workforce in-home health aide work, housekeeping and gardening, and other occupations. For some older Americans who need assistance but can live in the community with support, it is enough to make a difference. We estimate that institutionalisation rates in the year 2000 were about 10% lower than they would have been without the growth in the immigrant population since 1980.
More formally, we can think of caregiving as a service that can be produced with a mix of physical and technological capital, specialised labour, and less-educated labour. Institutional caregiving makes more use of capital and specialised labour, whereas home care disproportionately uses other forms of labour. Clemens et al. (2018) show that immigration can alter the choice of production technologies in the agricultural sector. Here, we imagine that an increased supply of less-educated labour makes it more cost-effective to care at home for some older individuals on the margin rather than using a capital-intensive approach in a nursing home.
Even as immigration lowers institutionalisation rates, it also improves the quality of care for those who do live in institutions. Furtado and Ortega (2020) show evidence of fewer falls among nursing home residents when immigration is higher, particularly in competitive markets where staffing levels are more responsive to supply. This result is consistent with earlier work showing that tight labour markets worsen mortality in nursing homes (Miller et al. 2009), presumably due to staffing shortages.
The potential effects ripple beyond the living arrangements of the elderly themselves. The needs of an elderly parent may affect the activities of their adult children. A 2020 study in Austria finds that negative health shocks among the elderly reduce the labour supply of their adult children, particularly for daughters and for those who live nearby (Frimmel et al. 2020). A liberalisation of the formal care market in 2007 that allowed more migrant care workers into the country muted the effects of health shocks on adult children's labour supply. Another study in Italy finds that increased immigration allows women, particularly those with elderly parents, to retire later in life (Perri et al. 2015).
The leading edge of the baby boom turns 76 in 2022, and, as shown above, age-related disability increases non-linearly after age 80. The caregiving workforce will have to dramatically expand to meet this need over the next decade. Given that most older Americans would prefer to live in the community where possible, it is important to consider what may help them to actualise those preferences. Increasing the supply of less-educated labour by expanding immigration is one way to facilitate ageing in place, while also easing the burdens of caregiving that fall on adult children and improving the quality of institutional care.
This article first appeared on www.VoxEU.org on February 22, 2022. Reproduced with permission.




